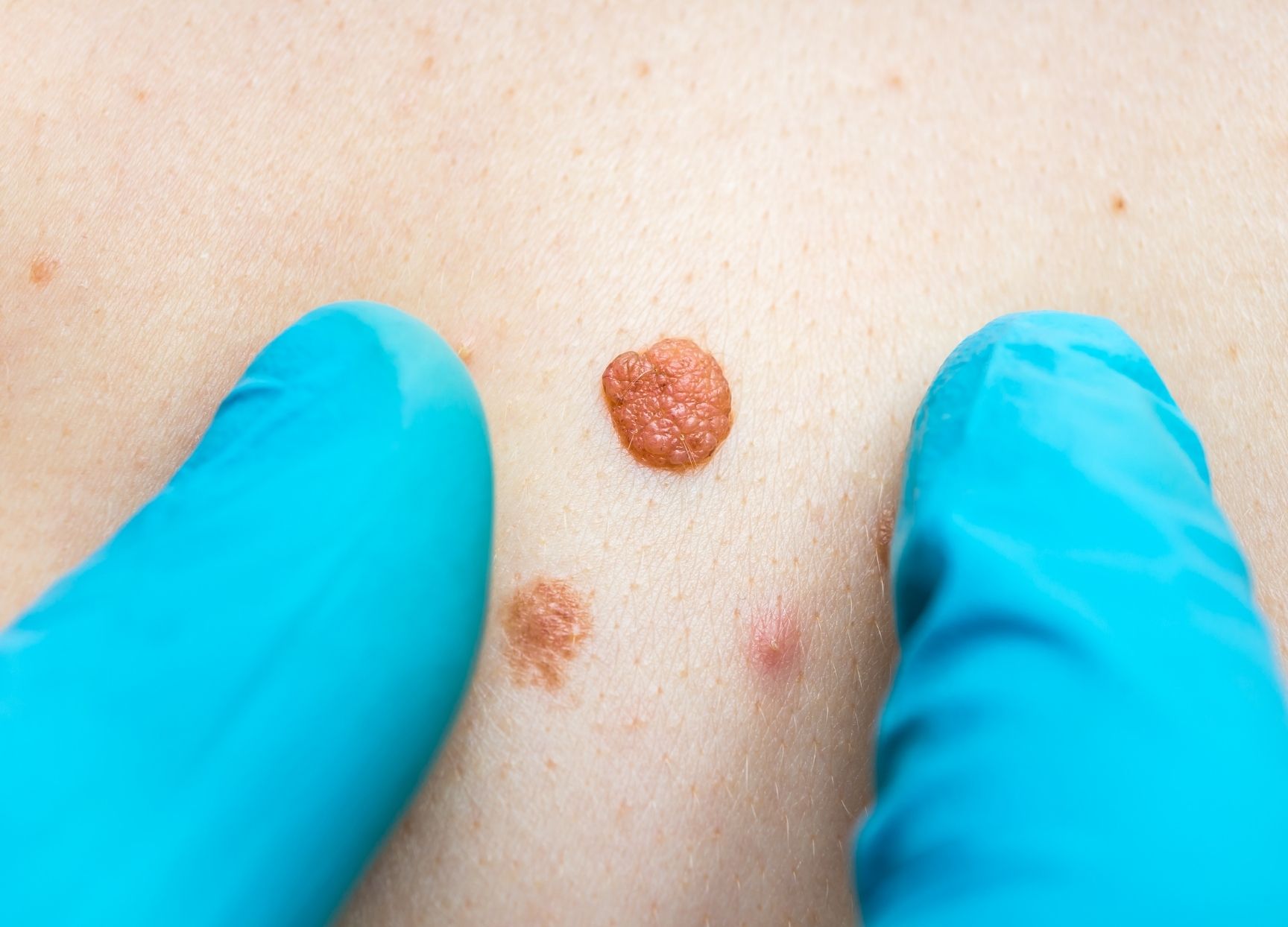
Skin cancer is the most common form of cancer in humans and hence it is important to be aware of the condition, which we highlight during our skin cancer awareness month campaigns. It consists of a malignant growth, which usually develops in the outermost layer of the skin called the epidermis, meaning that a tumour is generally clearly visible. It primarily develops on areas of skin that are exposed to the sun such as the scalp, face, ears, lips, neck, chest, arms and hands. Skin cancer rarely spreads beyond the skin, apart from malignant melanoma (See below).
The epidermis contains three different types of cells:
- Squamous cells – just below the outer surface.
- Basal cells – below the squamous cells, these produce new skin cells.
- Melanocytes – these are in the lower part of the epidermis and give the skin it’s normal colour.
There are three main types of skin cancer:
- Squamous cell carcinoma – about 25% of all skin cancers, this is quite aggressive but rarely spreads to local lymph nodes
- Basal cell carcinoma – 70-75% of all skin cancers, this is the most common. It progresses very slowly but can be destructive to local cells.
- Malignant melanoma – 1-5% of skin cancers – this is a very aggressive tumour and is very often seen with regional and / or distant metastasis (see below)
Skin cancer is more likely to develop in people that show the following risk factors:
- Lighter natural skin colour
- Family or personal history of skin cancer
- Exposure to the sun
- A history of sun burns early in life
- Skin that burns, freckles, reddens easily or becomes painful in the sun
- Blue or green eyes
- Blonde or red hair
- Certain types and a large number of moles

Preventing skin cancer
Ultraviolet radiation that is found in sunlight and tanning beds/lamps is the best-known cause of skin cancer, with both ultraviolet A (UVA) and ultraviolet B (UVB) contributing to skin cancer development. Therefore, the best way to prevent skin cancer is to protect yourself from the sun by doing the following:
- Find shade, especially between 10am and 4pm when UV rays are strongest and most damaging.
- Cover up with clothing.
- Wear a wide brimmed hat to protect your head, face, ears and neck.
- Wear sunglasses that wrap around and block as close to 100% of both UVA and UVB rays as possible.
- Use sunscreen with both UVA and UVB protection of SPF 15 or higher
Warning signs of skin cancer
The most common warning sign is a change on the skin, particularly a new growth or a sore that doesn’t heal. Skin cancer might start as any of the following:
- A small, smooth, shiny, pale or waxy lump
- A firm red lump
- Sometimes the lump may bleed or form a crust
- A flat red spot that is rough, dry or scaly
- Rough red or brown scaly patches (known as actinic keratosis) can turn into squamous cell cancer

How is skin cancer diagnosed?
Various skin cancer screening options include:
Mole checks: a dermatologist will examine skin and use a dermatoscope to look at the networks in your moles more closely. They will determine if moles have any abnormalities or need further monitoring or removal.
Mole mapping: an advanced whole body 3D imaging system which captures the entire skin surface to map and monitor pigmented lesions, all in 10 seconds.
Dr Katie Lacy, one of our leading dermatologists, has taken a closer look at the clinical rationale behind mole mapping in detecting skin cancer.
If you have an area of skin that looks abnormal, your doctor will remove all or part of the growth to perform a biopsy. They send the tissue they have taken for a histopathologic examination to check for cancer cells. This is the only way to be certain if cancer is causing the abnormality in your skin.

Skin Cancer Treatments
The main goal when treating skin cancer is to completely remove or destroy the cancer without leaving too much of a scar. Treatment options will depend on the size and location of the cancer, the risk of scarring, your age, general health and medical history. These options include:
- Curettage and Electrodesiccation – In this procedure, your surgeon uses a spoon-shaped instrument called a curette to scoop out the cancer. They will then treat the area with an electric current to control any bleeding and destroy any remaining cancer cells at the edge of the wound (electrodesiccation). This is carried out under local anaesthetic and most patients will heal with a flat white scar.
- Mohs’ surgery – This is a special surgical technique used for skin cancer which aims to remove all of the cancerous tissue and as little healthy tissue as possible. It is especially helpful when the consultant doesn’t have a clear picture of the shape and depth of the tumour. It is necessary in less than 10% of cases.
- Cryosurgery – Certain small skin cancers and actinic keratosis can be treated using application of liquid nitrogen to freeze and kill the abnormal cells in a growth. Your doctor may need to perform more than one freezing to completely remove the growth. This procedure does not hurt but you may experience pain and swelling when the area starts to thaw. You may develop a white scar after treatment.
- Laser therapy – For cancers that only involve the outer layer of skin, this procedure uses a narrow beam of light to remove or destroy the cancer cells. Photodynamic therapy is the process of using a combination of laser light and drugs that make the cells sensitive to light to destroy cancer cells.
- Excision surgery – this is the main treatment used for skin cancer, during which your surgeon will usually remove the tumour with safety margins of 4-7mm, depending on its size and location. The wound will then be closed, possibly covered by adjacent skin (flaps) or a piece of healthy skin from another part of your body, or it may be left open to heal by itself.
- Radiation therapy – This is mainly used for cancers that occur in areas that make it difficult to treat them with surgery. Several treatments may be needed to fully destroy all of the cancer cells. It may cause a rash or make the skin appear dry or red.
- Topical chemotherapy – This involves applying anti-cancer drugs to the skin in the form of a cream or lotion and is an effective treatment for actinic keratosis and very limited superficial cancers. It is common for this treatment to result in intense inflammation but not usually scarring.
Learn more about how cancerous moles are treated.
Meet one of our experts