Dr Emma Craythorne
Consultant Dermatologist
Specialist expertise: Skin Cancer, Skin Scarring, General Dermatology, Cosmetic Dermatology, Dermatology, Reflectance Confocal Microscopy, Laser Surgery, Burns.
Acne can affect a huge number of people at various ages, and there are a range of different types of the condition. Dr Emma Craythorne and Dr Rachael Morris-Jones, both Consultant Dermatologists and acne specialists at OneWelbeck Skin Health & Allergy, have put together a comprehensive guide to acne, what causes it and what the treatment options are.
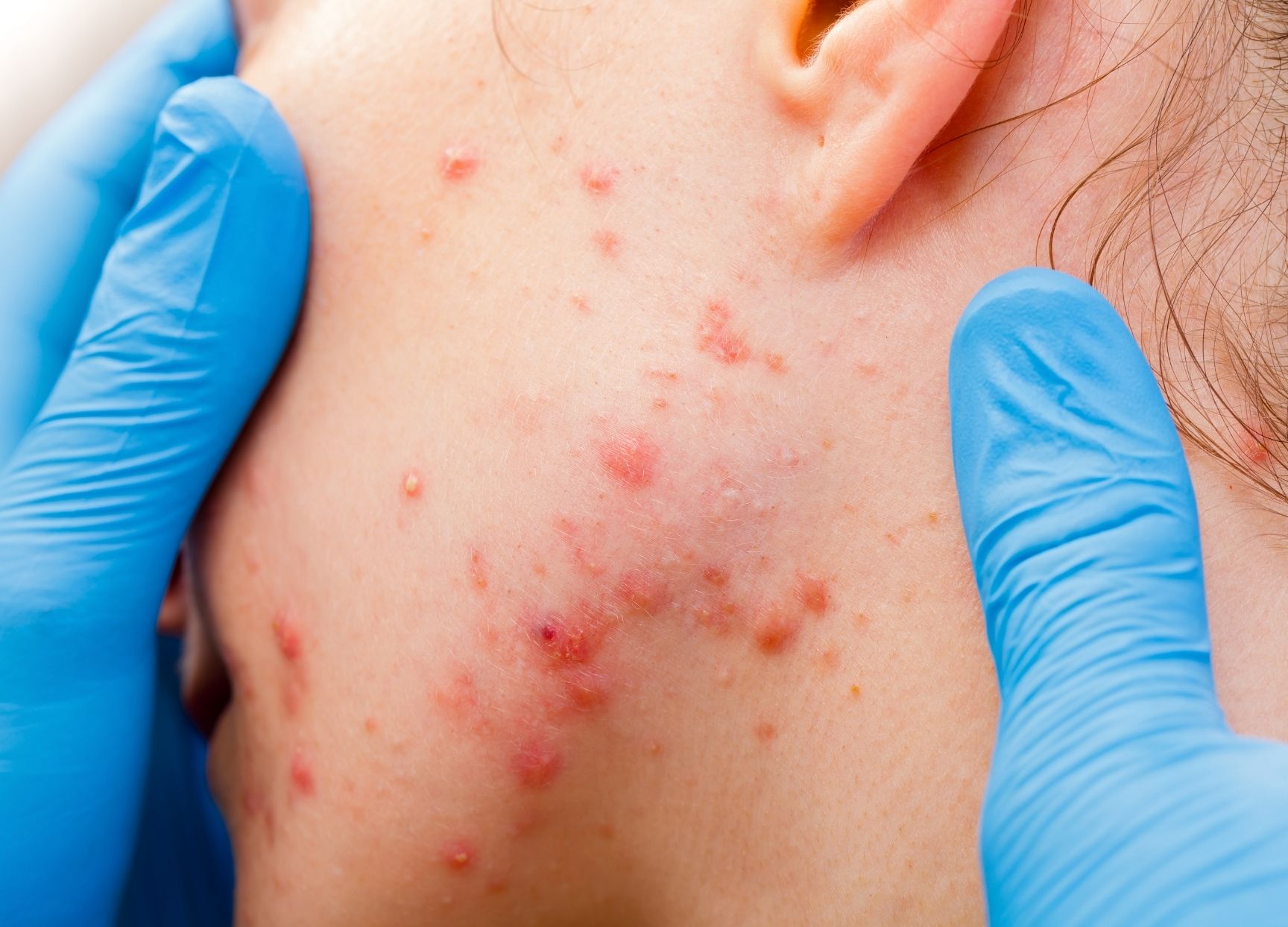
Some people refer to acne as ‘spots’ or ‘outbreaks’. These are blemishes on the skin that develop from blockage and enlargement of the oil glands in the skin (sebaceous glands). This leads first to comedones (whiteheads and blackheads) inflammatory papules and pustules (pus spots) and deeper lumps in the skin called cysts.
It can run in the family (genetically linked), hormone imbalances can play a role, increased stress levels (which causes inflammation around the oil glands) can trigger or exacerbate it, and mask-wearing (covering the skin on the face) can lead to clogging of the pores leading to acne for the first time or making current acne worse. Heat and sweat can exacerbate acne, particularly on the back.
It’s not thought that any individual foods trigger acne but some people may notice that chocolate or highly processed foods may make their acne worse. Acne is not contagious (you can’t give it to anyone) and its go nothing to do with being ‘unclean’ or not washing the skin properly.
About 80% of us will get some sort of acne during our lifetime from babies (rare) to adolescents (common) to adults up to the age of 50 years. So, a huge range of ages. Its slightly more common in males (40% between the ages of 18-19 years) than females (peak age 16-18 years).
Acne tends to occur in the oiliest skin areas, such as the face (especially on the cheeks, chin, forehead), neck below the jawline, upper and lower back areas and chest. The T-zone (forehead, nose and chin) can particularly be affected by overproduction of oil in the skin leading to acne.
Topical treatments – preparations that are applied directly to the skin affected include lotions, gels, serums, creams. These have different types of active ingredients in them including antibiotics (kill bacteria, reduce inflammation), retinoids (remove dead skin to unblock comedones), benzoyl peroxide (kills bacteria, reduces inflammation, and unplugs pores), azelaic acid (kills bacteria and removes dead skin cells). Medicated preparations are usually applied at night and can cause some redness, peeling and dryness due to the way they work to unblock the skin pores.
Tablet treatments – oral antibiotics usually erythromycin (for children less than 12 years of age), tetracycline antibiotics (main ones that are effective), hormonal treatments (in females) such as oral contraceptive pills, spironolactone, oral retinoids such as isotretinoin (Roaccutane).
Light treatments – handheld light devices (can help to kill bacteria in the skin), N-lite treatment.
Physical treatment – comedones can be extracted by someone skilled in removing them, occasionally large painful inflamed acne cysts can be injected with steroid to help shrink them more quickly.
It is common to get red marks or brown marks at the site of previous acne spots, these are not usually permanent marks and fade slowly by themselves with time (months or years usually). You can use preparations to help fade the marks more quickly which may be recommended by your dermatologist.
Patients usually have a variety of scars following inflammatory acne, each acne lesion can leave a different type of scar. There are two basic types of scars depending on whether there is a net loss or gain of collagen:
There are multiple different modalities used to treat acne scarring and this is because each scar type does well with its own particular scar treatment. Each scar type is mapped and the optimal treatment in a staged approach is chosen dependent upon scar type, skin colour and down time. This form of acne scar management focuses on the patient and their particular scar types.
Surgical Approach – can be used to treat tethers, holes and dips within the skin. Surgical excision, subcision and punch techniques are employed.
Resurfacing Approach – this is used to tighten and even the surface of the skin and is performed with lasers, micro-needling radio-frequency, TCA CROSS acids and pulsed light.
Colour Change Approach – used to even out redness or pigment changes, lasers or topical creams are used.
Here at OneWelbeck, we have a team of specialists, state of the art facilities and diagnostics, and highly competitive financial packages for self-funding patients as well as those with private health care.
Dermatology AllergyWritten by Dr Emma Craythorne, Consultant Dermatologist and skin scarring specialist at OneWelbeck Skin Health & Allergy, and Dr Rachael Morris-Jones, Consultant Dermatologist and acne specialist at OneWelbeck Skin Health & Allergy.