
Dr Simon Sporton
Specialist expertise: Heart Rhythm Disturbances including Atrial Fibrillation, Pacing and Syncope, Heart Rhythm Disorders, Cardiology, Atrial Fibrillation Ablation, Heart Health, Pacemakers, Arrhythmias, Complex Devices.
Written by Dr Simon Sporton, Consultant Cardiologist at OneWelbeck Heart Health, who takes a closer look at the procedure.
Catheter ablation is a treatment in which a specific area of the heart is frozen (cryoablation) or heated (radiofrequency ablation) in order to prevent the generation or spread of abnormal electrical impulses that cause an abnormal heart rhythm. Catheters are long, thin tubes that are passed to the heart by way of a vein, or occasionally artery, in the groin. These catheters are used to make electrical recordings from the heart and to deliver ablation energy. Like all medical procedures, catheter ablation carries a risk of complications. The overall risk of a complication and the risk of individual complications varies depending on the heart rhythm being treated and on certain patient-related factors. Your consultant will discuss these with you, together with the risks and benefits of other treatment options such as drugs.
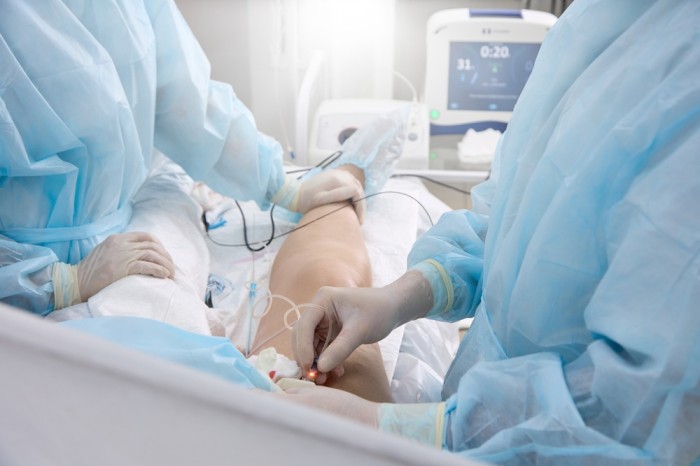
Some superficial bruising is expected on the groin, where the catheters are inserted into blood vessels. The bruising may spread over the next few days but then, like all bruises, changes colour and then fades.
Occasionally a swelling develops in the groin, which might require evaluation with an ultrasound scan. Usually this is due to a collection of blood under the skin known as a haematoma. This should resolve without specific treatment. Less commonly the swelling is due to a weakening in the wall of the femoral artery known as a pseudoaneurysm.
This is not dangerous but would typically need to be injected with a substance called thrombin, which causes the pseudoaneurysm to clot off or, occasionally, repair by a vascular surgeon.
A rare complication is a retroperitoneal haematoma, where bleeding occurs around the blood vessels as they run through the back of the abdomen. This is uncomfortable and may need to be managed in hospital, but typically resolves without specific treatment.
The pericardium is the sac that surrounds the heart. Pericardial effusion is an accumulation of fluid within the pericardium. The most common cause of pericardial effusion relating to catheter ablation is leakage of blood from the heart into the pericardium, which typically occurs during or immediately after the procedure. A less common cause is an inflammatory reaction, which may occur after a few days. Many pericardial effusions will resolve without specific treatment but in certain cases a drain will need to be inserted under the ribs and, uncommonly, heart surgery may be required. Recovery is typically complete, with no long-lasting effects.
Catheter ablation procedures that involving passing catheters to the left side of the heart carry an inherent small risk of stroke as that side of the heart is in direct communication with the rest of the body, including the brain. During a catheter ablation procedure in the left heart an anticoagulant (‘blood thinning’) drug called heparin is given to minimise the likelihood of blood clot forming. In addition, catheter ablation of atrial flutter and atrial fibrillation typically involves pre- and post-treatment with an oral anticoagulant drug, which is usually taken without interruption at the time of the procedure.
Catheter occasion may occasionally result in damage to structures close to the area of the heart that needs to be treated in order to cure the heart rhythm problem. The heart’s normal electrical conduction system (the atrioventricular node and His bundle) may occasionally by affected by catheter ablation for supraventricular tachycardia. If this does not recover, it may be necessary to fit a pacemaker. The right phrenic nerve, which supplies the right side of the diaphragm, may occasionally be affected by catheter ablation for atrial fibrillation. This may cause breathlessness on exertion, which may take up to a few months fully to recover. Cases of permanent phrenic nerve palsy have been reported. Rarely, damage can occur to the coronary arteries as a result of catheter ablation, in extreme cases resulting in damage to the heart muscle (‘myocardial infarction’). An extremely rare complication of catheter ablation of atrial fibrillation is the formation of a fistula (abnormal connection) between the left atrium of the heart and the oesophagus (‘gullet’).
Catheter ablation procedures may involve the use of x-rays. Non-fluoroscopic mapping systems are used in many ablation procedures. These systems bring many benefits, including the ability to perform catheter ablation using minimal, and sometimes no x-ray fluoroscopy.

Here at OneWelbeck, we have a team of cardiology specialists, state of the art facilities and diagnostics, and highly competitive financial packages for self-funding patients as well as those with private health care.
Contact UsDr Simon Sporton is a consultant cardiologist and electrophysiologist at OneWelbeck Heart Health, specialising in the investigation and management of heart rhythm disorders.