Mr Lee Parker
Consultant Foot and Ankle Surgeon
Specialist expertise: Foot and Ankle Conditions, Orthopaedics, Foot & Ankle, Bunions, Hammer Toe, Sports Injuries, Achilles Tendon Surgery.
Bunions are one of the most common forefoot complaints, but what are they and how should they be managed?

Bunions are one of the most common forefoot complaints, but what are they and how should they be managed?
A bunion is a swelling on the inside of the foot caused by mal-alignment of the bones making-up the Great toe. The medical term for this is “hallux valgus”.
Lee Parker, Consultant Orthopaedic Surgeon, explains when an operation should be considered and helps to dispel some of the myths around the treatment of this condition.
As with many medical conditions, a bunion can be caused by different factors, often acting together. Bunions do however run in families and tend to be more common in women, especially those with ligament laxity. Shoes that squeeze the toes together or place undue stress on the forefoot by having a high heel can cause the Great toe to deviate over time and occasionally an injury to the foot may cause a bunion.
There are several different designs of toe-splint marketed with the promise of preventing deformity progression or even correcting the bunion altogether. These splints tend to be very bulky and extended wear for many hours is suggested. Unfortunately the marketing claims are unsubstantiated and there is no evidence that these splints work. The only role for a splint is after surgery when a week or two of extra protection of the healing foot may be desired.
Toe separators are different.- They are usually made from silicone and can be worn inside shoes. They can be useful in patients who wish to avoid surgery altogether or who are too frail for an operation and don’t mind the feeling of the silicone inside their shoe.
Many patients have bunions which do not cause pain or limit their physical activity to any degree. If you develop pain, it is advisable for you to choose footwear that accommodates the bunion.- A wider-fitting shoe with a soft upper is ideal. Having a bunion does not mean you cannot wear Stiletto heels but it would be better to spend less time in them overall and to look for shoes with a lower heel. If you enjoy running, an “over-pronation” trainer or a running shoe with an arch support can be helpful to relieve pressure on the bunion.
Commercially-available bunion pads and plasters may help if you are beginning to get pain over the bunion or a build-up of hard skin.
Many people have bunions that do not give significant symptoms and do not progress beyond a mild deformity. Bunions can however occur alongside other deformities in the foot. As a hallux valgus deformity progresses, the Great toe’s role in weight-transmission is passed across onto the ball of the foot. You may notice a build-up of hard skin under the ball of the foot as this happens. Eventually, the increased pressure under the forefoot can result in the development of a hammer-toe deformity of the second toe. Sometimes, usually with a severe deformity, bursitis or even ulceration can occur over the bony prominence underneath the skin of a bunion.
If you experience regular discomfort in your foot, not helped with any of the measures above, if you have had episodes of inflammation/bursitis or ulceration over the bunion or if you are developing problems with other toes such as hammering or crossing-over then you should see an orthopaedic consultant to discuss surgical treatment options. If you are concerned about your bunion but it is not causing you pain we are happy to see you to offer advice but surgery on asymptomatic bunions or cosmetic corrections would not be recommended.
You will be offered an appointment at your convenience for a careful history and clinical examination of your feet to be carried-out. If your symptoms indicate it, you will undergo a standing X-ray or CT scan of your foot. Following this, you will be taken through the options for managing your bunion- both non-surgical and surgical treatments.
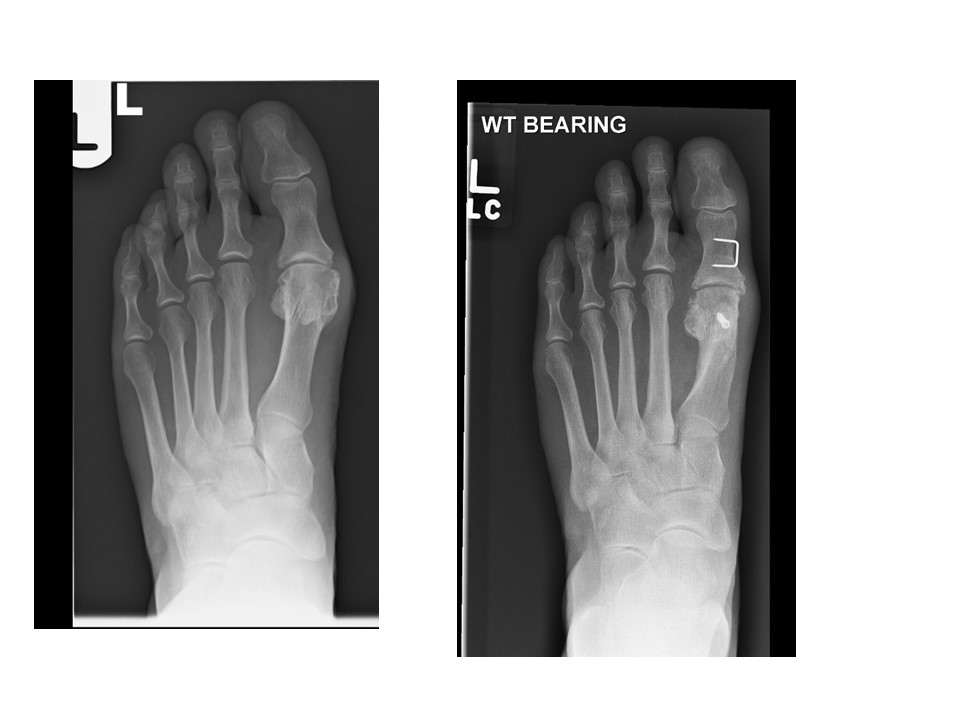
A bunion operation is a very common day surgery procedure and involves straightening the Great toe by performing small bone saw-cuts and strengthening lax soft tissues around the toe. The cuts in the bone are called osteotomies and are held in place with small internal screws or occasionally a staple (before and after surgery X-rays are shown below). Bulky bandages are worn on the foot for two weeks after the operation and you do not usually require a plaster cast. Weight-bearing in a surgical shoe is allowed immediately after the operation and continues for six weeks. Crutches are not usually required.
Bunion surgery can be carried out under general anaesthetic (with you unconscious and unaware of pain) or under regional anaesthesia (with you awake and unaware of pain) or a combination of techniques.
After discharge we advise you to keep your foot elevated for most of the time and rest at home for the first two weeks. Simple pain killers, often a combination of an anti-inflammatory and paracetamol or codeine will be needed regularly for the first few days after the operation and then tapered-off as pain improves. The most important form of pain relief comes from elevation to reduce swelling in the foot.
Resumption of normal activities after forefoot surgery is different for every patient. At your six week clinic appointment you will be asked to disregard your offloading surgical shoe to start putting pressure through your forefoot in a wide-fitting shoe. Over the course of several weeks you will gain confidence as your pain improves. Swelling however can persist for several months after bunion surgery and is normal. Physiotherapy can help you to regain strength and movement in your foot and aid with transition to normal walking in your usual footwear.
If you have a manual job requiring you to spend significant time on your feet you will need about 8-10 weeks off work but most patients with predominantly administrative jobs can return to work after 4-6 weeks.
When it comes to exercise, you will be advised by your orthopaedic surgeon when you can start exercise, however for most patients, upper-body exercises and cycling can begin after 6-8 weeks. Lower limb exercises and running should generally not be thought of as possible until after four to six months.
What is a bunion?
My mum and grandmother have bunions – does it run in families?
How effective are bunion splints?
Is there anything I can do with my shoes that may help?
What if I ignore the problem, is it likely to get worse?
When should I see an orthopaedic surgeon?
What does a bunion operation involve?
How long does recovery from surgery take?
When could I return to work and/or sport?
Here at OneWelbeck, we have a team of specialists, state of the art facilities and diagnostics, and highly competitive financial packages for self-funding patients as well as those with private health care.
OrthopaedicsMr Lee Parker is a Consultant Foot and Ankle Surgeon at OneWelbeck Orthopaedics. A well-known figure within his specialty, Mr Parker has extensive experience in managing foot and ankle trauma. His NHS base is at The Royal London Hospital, one of Europe’s largest trauma centres.