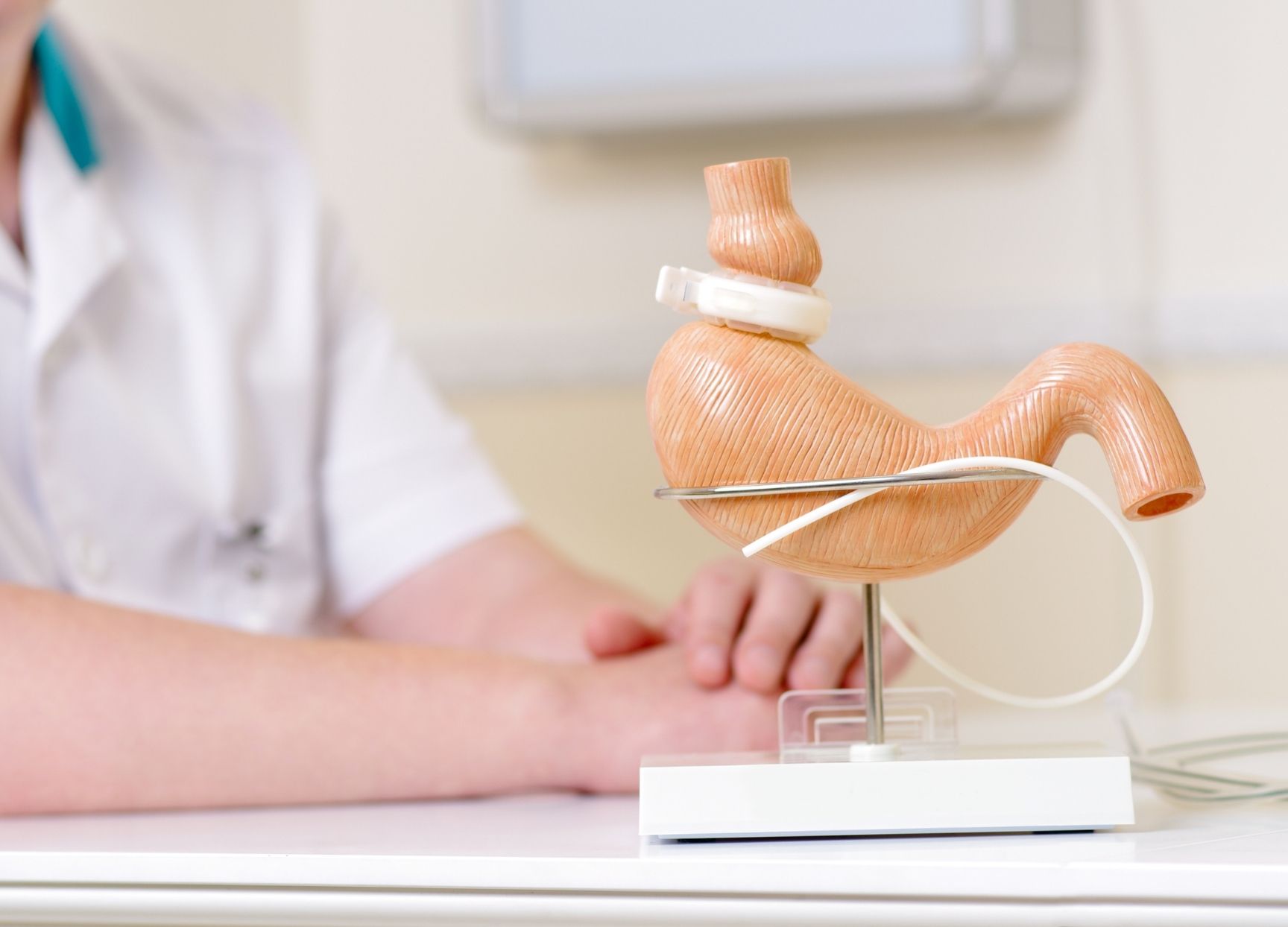
There are three main types of bariatric surgery:
Gastric band
A band is placed around the very top of the stomach to make you feel more full when you eat and help reduce portion sizes. As this does not cause the hormonal changes seen with the other bariatric operations, it can be harder to achieve and maintain sufficient weight loss.
Sleeve gastrectomy
The surgeon will make a narrow tube out of your stomach which results in increased fullness after eating small portions but also there is a modest increase in the gut hormones that encourage weight loss. Typical weight loss seen with a sleeve gastrectomy is 50-60% of excess body weight.
Gastric Bypass
This is the most effective form of bariatric surgery achieving 60-70% excess body weight loss. Improvement or remission from Type 2 diabetes has been demonstrated in 92% of all clinical trial patients between 2003-2012 (1 JAMA meta-analysis, 2014).
This operation involves the surgeon creating a small pouch of stomach, then makes a cut in the small intestine and bring the lower part of the small intestine to attach to the stomach pouch. Food then passes from the mouth to the stomach pouch and then to the lower small intestine which reduces the amount of food and calories absorbed. The remaining intestine is left intact to enable digestive juices to enter the gut.
Both gastric bypass and sleeve gastrectomy patients require lifelong vitamin replacement however it is often possible to stop many diabetes and blood pressure medications post-operatively.
Bariatric surgery is covered by a limited number of insurance companies; it is important to confirm the details of your insurance policy.
To proceed to bariatric surgery, patients need to follow the “golden rules” bariatric diet designed to optimise weight loss and address nutritional deficiencies and complications such as dumping syndrome that can occur post bariatric surgery. This includes high protein intake, carefully controlled sugar and carbohydrate intake and to avoid fizzy drinks and smoking. Many bariatric surgeons will give patients a weight loss target to achieve prior to their surgery; this can be achieved through dietary changes, meal replacement diets and medications such as Saxenda (liraglutide) or semaglutide can be helpful to encourage weight loss. These medications are not needed after bariatric surgery as the body produces high levels of its own version of these hormones.